Top Hospitals for Neuro / Spine View All 
Best Doctors for Neuro / Spine View All 
Director & Head- Neuro & Spine Surgery
CONSULTS AT EXPEREIENCE :19+ years SURGERIES :
10000+
Treatment Price on request
Free Text ConsultTreatment Price on request
19+ years SURGERIES :
10000+ TREATMENT COST
Treatment Price on request
Executive Director - Neuro Spine Surgery
CONSULTS ATFortis Memorial Research Institute, Gurgaon
EXPEREIENCE :20 years SURGERIES :
7000+
Treatment Price on request
Free Text ConsultTreatment Price on request
20 years SURGERIES :
7000+ TREATMENT COST
Treatment Price on request
Chairman - Neuro Spine Surgery
CONSULTS ATFortis Memorial Research Institute, Gurgaon
EXPEREIENCE :23+ years SURGERIES :
10000+
Treatment Price on request
Free Text ConsultTreatment Price on request
23+ years SURGERIES :
10000+ TREATMENT COST
Treatment Price on request
Orthopedics & Spine Surgeon
CONSULTS ATSCI International Hospital, New Delhi +1
EXPEREIENCE :26 years SURGERIES :
NA
Treatment Price on request
Free Text ConsultTreatment Price on request
26 years SURGERIES :
NA TREATMENT COST
Treatment Price on request
Senior Consultant - Spine & Deformity Correction
CONSULTS AT EXPEREIENCE :17 years SURGERIES :
2000+
Treatment Starting at $5,000
Free Text ConsultTreatment Starting at $5,000
17 years SURGERIES :
2000+ TREATMENT COST
Starting at $5,000
Senior Director – Neurosurgery
CONSULTS ATMax Super Speciality Hospital, Patparganj
EXPEREIENCE :21 years SURGERIES :
8000+
Treatment Price on request
Free Text ConsultTreatment Price on request
21 years SURGERIES :
8000+ TREATMENT COST
Treatment Price on request
Testimonials
View All 
- Treatment : Brachial Plexus
- Hospitals : Indraprastha Apollo Hospital
- Treatment : Treatment Unknown
- Hospitals : Fortis Hospital, Noida
- Treatment : Cervical Decompression with Fixation Surgery
- Hospitals : Fortis Memorial Research Institute, Gurgaon
- Treatment : Treatment Unknown
- Hospitals : Fortis Hospital, Noida
- Treatment : Brain Tumor Surgery
- Hospitals : Fortis Hospital, Noida
- Treatment : Brain Tumor Surgery
- Hospitals : Fortis Memorial Research Institute, Gurgaon
- Treatment : Brain Tumor Surgery
- Hospitals : Gleneagles Global Health City, Chennai
- Treatment : Discectomy and Fixation
- Hospitals : Fortis Memorial Research Institute, Gurgaon
Related Blogs
View All 
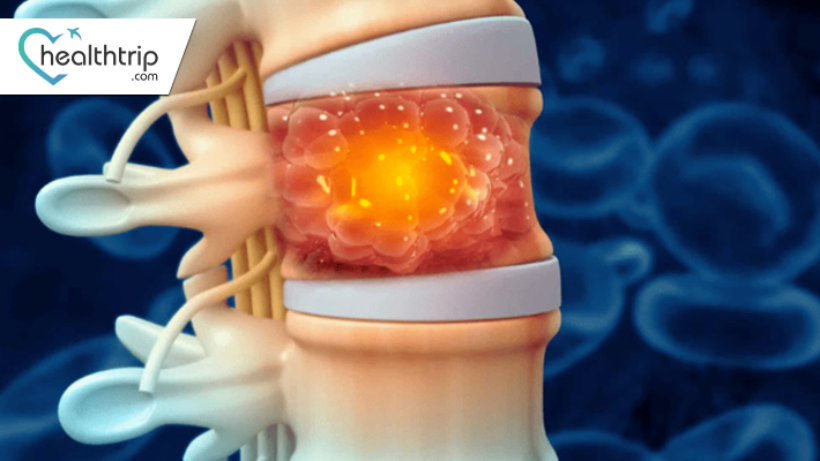
Spinal Cord Tumors: Types, Symptoms, and Treatment
The human spine, a complex and vital component of our central nervous system, can occasionally be afflicted by the presence of tumors that impact the spinal cord. Spinal cord tumors, diverse in their forms and characteristics, pose unique challenges to individuals and healthcare providers alike. Understanding these tumors requires a nuanced exploration encompassing their types, demographic patterns, symptoms, diagnostic methods, and available treatment options. This journey of comprehension is essential not only for those directly affected but for the broader medical community, as it opens doors to timely interventions, improved prognoses, and ongoing advancements in research. In this exploration, we delve into the intricate landscape of spinal cord tumors, aiming to shed light on their intricacies and significance in the realm of healthcare.Spinal Cord Tumor: - A spinal cord tumor is an abnormal growth of cells within or near the spinal cord. These tumors can be either benign (non-cancerous) or malignant (cancerous), and they may affect the spinal cord or the surrounding structures.Understanding spinal cord tumors is crucial as they can impact the delicate and vital functions of the nervous system. These growths can lead to a range of symptoms, affecting a person's mobility, sensation, and overall well-being. By gaining insights into these tumors, we can improve early detection, enhance treatment outcomes, and ultimately enhance the quality of life for affected individuals.Types of spinal cord tumorsBy location:1. Intramedullary Tumors:These tumors develop within the spinal cord itself, intricately intertwined with the nerve tissues.Intramedullary tumors originate from cells within the spinal cord and can affect the delicate neural structures. They often infiltrate the surrounding tissues, making surgical removal challenging.Gliomas, ependymomas, and hemangioblastomas are common types of intramedullary tumors.Due to their location, intramedullary tumors may disrupt normal neural function, leading to symptoms such as motor weakness, sensory changes, and pain.2. Extramedullary Tumors:These tumors grow outside the spinal cord but within the spinal canal, the protective bony structure surrounding the cord.Extramedullary tumors usually originate from the supportive tissues surrounding the spinal cord, such as the meninges or nerve roots. They may push on the spinal cord, causing symptoms by compression or infiltration.Meningiomas, schwannomas, and neurofibromas are common types of extramedullary tumors.While extramedullary tumors are outside the spinal cord tissue, they can still exert pressure on neural structures, leading to symptoms like back pain, weakness, or sensory changes. Surgical removal is often more feasible for these tumors compared to intramedullary tumorsThe most common type of spinal cord tumor is an intramedullary tumor, which is a tumor that grows within the spinal cord itself.The second most common type of spinal cord tumor is an extramedullary tumor, which is a tumor that grows outside of the spinal cord.By type of cells:A. Meningiomas: - Meningiomas are typically slow-growing tumors that arise from the meninges, the protective layers surrounding the spinal cord and brain. They are often benign and may cause symptoms by pressing on the spinal cord or nerve roots.B. Ependymomas: - Ependymomas develop from the ependymal cells lining the spinal cord's central canal. These tumors can occur at any age and may vary in aggressiveness. Symptoms are often related to the location and size of the tumor.C. Astrocytomas: - Astrocytomas originate from astrocytes, star-shaped cells that provide support to nerve cells. These tumors can be either low-grade or high-grade, and their effects depend on their location along the spinal cord.D. Schwannomas: - Schwannomas arise from Schwann cells, which produce the protective covering (myelin) around nerve fibers. These tumors are usually benign and can affect nerves in the spinal cord, causing pain, weakness, or numbness.E. Other Rare Types: - Various other rare types of spinal cord tumors exist, such as hemangioblastomas, gliomas, and lipomas. While less common, these tumors may present unique challenges in terms of diagnosis and treatment due to their rarity and diverse characteristics.Symptoms and SignsA. Back Pain:Persistent or severe pain in the back, often localized to the region where the tumor is affecting the spinal cord.B. Motor Weakness: Gradual or sudden loss of strength and coordination in the limbs, potentially leading to difficulty walking or performing daily activities.C. Sensory Changes: Altered sensations, such as tingling, numbness, or a "pins and needles" feeling, in areas served by the affected nerves.D. Loss of Bladder or Bowel Control: Inability to control urinary or bowel functions, which may indicate pressure on the nerves controlling these bodily functions.E. Other Neurological Symptoms: There are various neurological symptoms, including difficulty with balance, changes in reflexes, muscle spasms, and, in some cases, difficulty swallowing.Causes of Spinal Cord TumorsMen are slightly more likely than women to develop spinal cord tumors.A. Genetic Factors: Family history of spinal cord tumors or certain genetic syndromes that increase the risk.B. Environmental Factors: Exposure to certain environmental toxins or substances that may contribute to the development of tumors.C. Radiation Exposure: Previous exposure to ionizing radiation, either for medical purposes or other reasons, as a potential risk factor.D. Other Risk Factors: Factors such as age, gender, and certain medical conditions that may increase the likelihood of developing spinal cord tumors.Diagnosis of Spinal Cord TumorsThe diagnosis of spine tumors is a multi-step process that combines clinical evaluation with advanced imaging and laboratory techniques. Given the potential implications of a spine tumor, both benign and malignant, accurate diagnosis is paramount to guide treatment decisions and predict outcomes.Medical History and Physical Examination:Initial Assessment: The diagnostic journey typically begins with a comprehensive medical history and physical examination. The physician will gather information about the onset, duration, and nature of symptoms, any prior medical conditions, family history of similar issues or genetic disorders, and potential exposure to risk factors. The physical examination will assess pain, tenderness, range of motion, neurological deficits, and any visible spinal deformities.Imaging Tests:MRI (Magnetic Resonance Imaging): This is often the first imaging test ordered for suspected spine tumors. MRI uses powerful magnets and radio waves to produce detailed images of the spine, including the spinal cord, nerve roots, and surrounding structures. It's particularly adept at visualizing soft tissue, making it invaluable for identifying and characterizing tumors.CT (Computed Tomography) Scan: While MRI is superior for soft tissue, CT scans provide detailed images of bone. This makes them especially useful for visualizing vertebral column tumors, assessing bone erosion, or planning surgical interventions.Bone Scan: If there's a suspicion of metastatic spread or if the origin of the tumor is uncertain, a bone scan might be ordered. This involves injecting a small amount of radioactive material into the bloodstream, which then accumulates in areas of abnormal bone growth. A special camera then captures images of these areas, highlighting potential tumor sites.Biopsy:While imaging can suggest the presence of a tumor and provide information about its size, location, and relationship to surrounding structures, a definitive diagnosis often requires a biopsy. In this procedure, a small sample of the tumor tissue is extracted, either surgically or using a needle guided by imaging. This sample is then examined under a microscope by a pathologist to determine the type of cells present, whether they're benign or malignant, and the grade of the tumor (how aggressive it looks). The results of the biopsy are crucial for treatment planning and prognostication. the diagnosis of spine tumors is a meticulous process that integrates clinical acumen with state-of-the-art diagnostic tools. Once a definitive diagnosis is made, a multidisciplinary team, including neurosurgeons, oncologists, radiologists, and other specialists, often collaborates to devise the best treatment strategy for the patient.Treatment Options of Spinal Cord TumorsA. Surgery:Surgical removal of the tumor, with the goal of alleviating pressure on the spinal cord and nerves. In some cases, complete removal may not be possible, and the surgeon may opt for debulking (partial removal) to improve symptoms.B. Radiation Therapy:Use of high-energy rays to target and destroy cancer cells. Radiation therapy is often employed when complete surgical removal is challenging or for tumors that are sensitive to radiation.C. Chemotherapy:Administration of drugs to kill or inhibit the growth of cancer cells. While less common for spinal cord tumors, chemotherapy may be considered in specific cases, particularly for malignant tumors or those that have spread from other parts of the body.D. Targeted Therapy:Use of drugs that specifically target certain molecules involved in the growth and survival of cancer cells. Targeted therapy is often tailored to the specific characteristics of the tumor.E. Rehabilitation:Physical therapy, occupational therapy, and other rehabilitation interventions to help patients regain strength, mobility, and functional independence after surgery or other treatments. Rehabilitation is crucial for improving overall quality of life.Risk FactorsA. Genetic Predisposition: Family history of spinal cord tumors or genetic conditions that increase susceptibility.B. Exposure to Certain Chemicals or Radiation: Occupational exposure to harmful chemicals or radiation, which may contribute to the development of spinal cord tumors.C. Age: Incidence increases with age, with certain types of spinal cord tumors more common in specific age groups.D. Other Medical Conditions: Presence of certain medical conditions or disorders that may elevate the risk of developing spinal cord tumors.Complications A. Neurological Deficits: Persistent impairment of neurological function, such as motor or sensory deficits, resulting from the tumor's impact on the spinal cord or nerve roots.B. Surgical Complications: Risks associated with surgical interventions, including infection, bleeding, and damage to surrounding structures.C. Treatment Side Effects: Adverse effects resulting from treatments such as radiation therapy or chemotherapy, which may include fatigue, nausea, and other temporary or long-term side effects.D. Impact on Quality of Life: The overall impact of spinal cord tumors on a person's daily life, including physical and emotional well-being, and the ability to perform routine activities.PrognosisThe prognosis, or the likely course and outcome of a disease, for individuals with spine tumors varies widely based on several factors.Factors Influencing Prognosis:Type of Tumor: Benign tumors, although they may cause significant symptoms, generally have a better prognosis than malignant ones.Location: Tumors located in areas that are difficult to access surgically or are near critical structures might have a more guarded prognosis.Size: Larger tumors, especially if they compress vital structures, might pose more significant challenges.Patient's Overall Health: Individuals with robust overall health may fare better in terms of treatment outcomes and recovery.Importance of Early Detection and Treatment: As with many medical conditions, early detection and intervention often lead to better outcomes. Smaller tumors that haven't caused irreversible damage or spread can often be treated more effectively.Prevention and Risk ReductionWhile it's not always possible to prevent spine tumors, certain measures can reduce the risk or aid in early detection.Regular Medical Check-ups: Routine health evaluations can help in the early identification of symptoms or signs suggestive of a spine tumor.Avoiding Exposure to Known Carcinogens: Reducing exposure to certain chemicals and high doses of radiation can potentially decrease the risk of spine tumors and other cancers.Genetic Counseling: For individuals with a family history of spine tumors or related genetic conditions, genetic counseling can provide insights into their risk and guide potential preventive measures.Spinal cord tumors encompass a diverse range of conditions with varied symptoms and outcomes. Understanding the key types, risk factors, and symptoms is vital for early detection and effective management. Timely diagnosis and appropriate treatment are essential for improving outcomes and minimizing complications. Early intervention can enhance the effectiveness of treatments and contribute to better quality of life. Ongoing research is critical for advancing our understanding of spinal cord tumors, developing innovative treatments, and improving overall patient care. Continued exploration of genetic, molecular, and treatment-related aspects will pave the way for future advancements in this field.
Best Hospitals for Spinal Cord Injury Treatment
IntroductionWelcome to a comprehensive guide on spinal cord injury treatment. Discover the best hospitals renowned for their expertise in spinal cord injury care. Our curated list features cutting-edge facilities equipped with advanced technology and a team of specialized professionals. From diagnosis to rehabilitation, these hospitals prioritize patient well-being, offering personalized treatment plans. Explore this guide to find the leading institutions dedicated to providing top-notch spinal cord injury treatment, ensuring the highest standards of medical care and support for those on the journey to recovery.Top Hospitals 1. Fortis Memorial Research Institute, GurgaonSector - 44, Opposite HUDA City Centre Gurgaon, Haryana - 122002, India, IndiaFortis Memorial Research Institute (FMRI) is a leading multi-specialty hospital in Gurgaon, India. It is one of the most popular destinations for medical tourists from all over the world, including those seeking hiatal hernia surgery.Fortis Memorial Research Institute (FMRI) in Gurgaon, India is one of the leading hospitals in the country for the treatment of spinal cord injuries. The hospital has a team of experienced and highly qualified neurosurgeons, neurologists, and other specialists who work together to provide comprehensive care for patients with spinal cord injuries.FMRI offers a wide range of spinal cord injury treatments, including:Emergency surgery: To stabilize the spine and prevent further damage to the spinal cord.Rehabilitation: To help patients regain as much function as possible and live independently.Pain management: To help patients control their pain and improve their quality of life.Clinical trials: To offer patients access to the latest and most promising treatments for spinal cord injuries.2. Max Healthcare SaketNew Delhi, Saket, IndiaMax Healthcare Saket, in New Delhi, India, is one of the leading hospitals in the country for the treatment of spinal cord injuries. The hospital has a team of experienced and highly qualified neurosurgeons, neurologists, and other specialists who work together to provide comprehensive care for patients with spinal cord injuries.Max Healthcare Saket offers a wide range of spinal cord injury treatments, including:Emergency surgery: To stabilize the spine and prevent further damage to the spinal cord.Rehabilitation: To help patients regain as much function as possible and live independently.Diagnosis: Max Healthcare Saket uses a variety of diagnostic tests to assess the severity of a patient's spinal cord injury and develop a personalised treatment plan.Surgery: The hospital's neurosurgeons perform a variety of surgeries to treat spinal cord injuries, including decompression surgery, stabilisation surgery, and fusion surgery.Rehabilitation: Max Healthcare Saket's rehabilitation team includes physiatrists, physical therapists, occupational therapists, speech therapists, and other specialists who work together to help patients regain as much function as possible. The rehabilitation team also helps patients adjust to their new lives and learn how to live independently.Pain management: The hospital's pain management team uses a variety of methods to help patients control their pain, including medication, physical therapy, and injections.Clinical trials: Max Healthcare Saket is a leading centre for clinical trials on spinal cord injuries. Patients at the hospital have the opportunity to participate in clinical trials of new and innovative treatments for spinal cord injuries.3. Jaypee Hospital Jaypee Hospital Rd, Gobardhanpur, Sector 128, Noida, Uttar Pradesh 201304, IndiaJaypee Hospital is a leading multi-specialty hospital in Noida, India. It has a team of highly experienced and skilled surgeons who specialise in hiatal hernia surgery. The hospital uses the latest techniques and equipment to perform the surgery safely and effectively.Jaypee Hospital in Noida, India, is a leading hospital for the treatment of spinal cord injuries. The hospital has a dedicated Institute of Neurosciences, which is equipped with the latest technology and facilities to diagnose and treat spinal cord injuries.The team of experienced and highly qualified neurosurgeons, neurologists, and other specialists at Jaypee Hospital work together to provide comprehensive care for patients with spinal cord injuries. The hospital offers a wide range of treatments, including:4. Manipal Hospital, New DelhiSector 6 adjoining MTNL building, Main Rd, Dwarka, New Delhi, Delhi 110075, IndiaManipal Hospital, New Delhi, is a leading hospital for the treatment of spinal cord injuries. The hospital has a dedicated Spine Centre, which is equipped with the latest technology and facilities to diagnose and treat spinal cord injuries.The team of experienced and highly qualified neurosurgeons, neurologists, and other specialists at Manipal Hospital work together to provide comprehensive care for patients with spinal cord injuries. The hospital offers a wide range of treatments,Manipal Hospital is also a leading centre for research on spinal cord injuries. The hospital's researchers are working to develop new and innovative treatments for this devastating condition.5. KIMS Hospital KIMS Hospitals in India offer comprehensive treatment for spinal cord injuries. The hospital has a team of experienced and highly qualified neurosurgeons, neurologists, and other specialists who work together to provide personalized care for each patient.The hospital also has a dedicated Spinal Cord Injury Center, which is equipped with the latest technology and facilities to diagnose and treat spinal cord injuries.

A Comprehensive Guide to Spondylolisthesis
What is Spondylolisthesis? Spondylolisthesis" is a medical term that refers to the condition where one vertebra in the spine slips forward or backward in relation to an adjacent vertebra. This displacement can occur for various reasons, such as degeneration of the spine due to aging, congenital abnormalities, stress fractures, or traumatic injuries. Spondylolisthesis is often categorized into different types based on its causes, such as dysplastic, isthmic, degenerative, traumatic, and pathological.Spondylolisthesis affects about 6% of the population worldwide.It is most common in people between the ages of 20 and 50.Spondylolisthesis is more common in females than in males.Types of Spondylolisthesis1. Dysplastic Spondylolisthesis:This type is characterized by a congenital defect in the formation of one or more vertebrae. It occurs during the developmental stage and is often present from birth. Structural abnormalities in the vertebrae contribute to the forward slippage.2. Isthmic Spondylolisthesis:This form results from a stress fracture, typically in the pars interarticularis—a small bridge of bone connecting the facet joints in the posterior spine. Repetitive hyperextension of the spine, common in certain sports or activities, can lead to this stress fracture and subsequent slippage.3. Degenerative Spondylolisthesis:Associated with the aging process, this type is characterized by the gradual deterioration of spinal structures. The intervertebral discs lose height and integrity, and the facet joints may undergo degenerative changes, contributing to the slippage of one vertebra over another.4. Traumatic Spondylolisthesis:This type is a result of a sudden injury or trauma to the spine, leading to vertebral displacement. Accidents, falls, or forceful impacts can cause fractures or dislocations that result in the misalignment of the vertebrae.5. Pathological Spondylolisthesis: Caused by an underlying disease affecting the spinal structures, this type is characterized by structural weakness due to diseases like osteoporosis, tumors, or infections. The compromised integrity of the spine increases the risk of vertebral slippage.Symptoms and Signs of SpondylolisthesisSpondylolisthesis can manifest with a variety of symptoms and signs, which may vary depending on the degree of vertebral slippage, the location of the affected vertebrae, and whether there is nerve compression. Here are the common symptoms and signs associated with spondylolisthesis:1. Lower Back Pain: Persistent lower back pain is a hallmark symptom of spondylolisthesis. The pain is often described as a dull ache that may worsen with activity, such as standing or walking, and improve with rest.2. Radiating Leg Pain: Some individuals may experience radiating pain that travels down one or both legs. This is often referred to as sciatica. The pain may be sharp, burning, or tingling in nature and can be accompanied by numbness or weakness in the legs.3. Tightness or Stiffness: Stiffness in the lower back and reduced flexibility can be a symptom of spondylolisthesis. Individuals may find it challenging to bend forward or backward comfortably.4. Change in Posture: Spondylolisthesis can alter a person's posture. Some individuals may develop a noticeable forward-leaning posture, particularly in more severe cases.5. Muscle Weakness: Weakness in the muscles of the legs or buttocks can occur when there is compression of spinal nerves. This weakness may result in difficulty walking, climbing stairs, or lifting objects.6. Numbness and Tingling: Numbness and tingling sensations, known as paresthesia, can affect the legs or feet. These sensations are often associated with nerve compression.7. Loss of Bowel or Bladder Control (Rare): In extremely severe cases of spondylolisthesis with significant spinal cord compression, there may be a loss of bowel or bladder control. This is a medical emergency and requires immediate attention.8. Fatigue: Chronic pain and discomfort associated with spondylolisthesis can lead to fatigue and a decreased ability to perform daily activities.9. Limited Mobility: Individuals with spondylolisthesis may experience limited mobility due to pain and stiffness. This can impact their ability to participate in physical activities or maintain an active lifestyle.Causes of Spondylolisthesis1: Congenital Spondylolisthesis: Some individuals are born with a congenital predisposition to spondylolisthesis. This occurs when there are abnormalities in the structure of the vertebrae, such as dysplasia (underdevelopment) of the facet joints or elongation of the pars interarticularis (a portion of the vertebra). Congenital spondylolisthesis is often present from birth but may not become symptomatic until later in life.2. Degenerative Spondylolisthesis: This is the most common type of spondylolisthesis and typically occurs in older adults. It is primarily caused by age-related changes in the spine, including:Degeneration of Intervertebral Discs: The intervertebral discs between the vertebrae can wear down over time, leading to a loss of disc height and stability.Facet Joint Arthritis: Arthritis of the facet joints, which are the small joints that connect adjacent vertebrae, can result in the slippage of one vertebra over another.Thickening of Ligaments: The ligaments that support the spine may thicken and contribute to instability.3. Traumatic Spondylolisthesis: Spondylolisthesis can develop as a result of acute injury or trauma to the spine. This may include fractures or dislocations of the vertebrae due to accidents or falls.4. Pathological Spondylolisthesis: In some cases, spondylolisthesis can occur due to underlying medical conditions or diseases, such as tumors, infections, or metabolic bone disorders, that weaken the vertebral structures.5. Isthmic Spondylolisthesis: This is a specific subtype of spondylolisthesis and is related to a defect in the pars interarticularis, a portion of the vertebra that connects the front and back parts. It can be caused by repetitive stress or microtrauma, particularly in activities that involve hyperextension of the lower back, such as gymnastics or weightlifting.6. Idiopathic Spondylolisthesis: In some cases, the exact cause of spondylolisthesis cannot be determined, and it is referred to as idiopathic. It may occur without an obvious congenital, degenerative, traumatic, or pathological cause.It's important to note that while these are the primary causes of spondylolisthesis, the condition's development can also be influenced by factors such as genetics, lifestyle, and mechanical stresses on the spine. Diagnosis of SpondylolisthesisI. Imaging StudiesA. X-raysPurpose:Visualize the alignment and structure of the vertebrae.Findings:Detection of slippage, fractures, or deformities.Grading the severity of spondylolisthesis.B. MRI (Magnetic Resonance Imaging)Purpose:Detailed imaging of soft tissues, discs, and nerves.Findings:Identifying nerve compression.Evaluating the condition of intervertebral discs.C. CT Scans (Computed Tomography)Purpose:Detailed cross-sectional images of the spine.Findings:Precise assessment of bony structures.Identification of fractures, defects, or abnormalities.II. Physical ExaminationA. Neurological TestsPurpose:Assessing nerve function and signs of compression.Tests:Reflex testing, muscle strength assessment, sensory examinations.Identifying any neurological deficits.III. Medical HistoryA. Identifying Risk FactorsPurpose:Understanding factors contributing to spondylolisthesis.Inquiries:Family history of spine-related conditions.Past injuries, activities, or occupations posing a risk.Treatment of SpondylolisthesisThe treatment of spondylolisthesis depends on several factors, including the severity of the condition, the presence of symptoms, the age and overall health of the individual, and the underlying cause. Here are the main treatment options for spondylolisthesis:1. Observation and Lifestyle Modifications:In cases of mild spondylolisthesis without significant symptoms, observation and lifestyle modifications may be sufficient.Lifestyle modifications may include avoiding activities that exacerbate symptoms, maintaining a healthy weight, and engaging in exercises that strengthen the core and back muscles to provide better spinal support.2. Physical Therapy:Physical therapy is often recommended to improve flexibility, strengthen muscles, and alleviate pain.Therapists can teach specific exercises and stretches tailored to the individual's condition to help reduce symptoms and improve mobility.3. Pain Management:Over-the-counter pain relievers, such as nonsteroidal anti-inflammatory drugs (NSAIDs), may be recommended to manage pain and inflammation.In some cases, corticosteroid injections into the affected area can provide temporary pain relief.4. Bracing:Bracing may be considered for individuals with spondylolisthesis to provide additional support to the spine.Braces are typically used for a limited time, such as during periods of increased pain or when engaging in physical activities.5. Surgical Intervention:Surgery is usually reserved for severe cases of spondylolisthesis that do not respond to conservative treatments or when there is spinal instability, neurological symptoms, or significant pain.Common surgical procedures for spondylolisthesis include:Spinal Fusion: This procedure involves fusing two or more vertebrae together to stabilize the spine and prevent further slippage. Bone grafts or implants may be used.Decompression Surgery: If nerve compression is a significant issue, decompression surgery may be performed to relieve pressure on the affected nerves.Laminectomy: In some cases, a laminectomy may be necessary to remove part of the lamina (the bony arch of the vertebra) to relieve pressure on the spinal cord or nerves.The choice of surgical procedure depends on the individual's specific condition and the surgeon's recommendations.6. Rehabilitation and Recovery:After surgery, individuals will typically undergo a period of rehabilitation to regain strength and mobility.Physical therapy and post-operative care are essential for a successful recovery.7. Regular Follow-Up:Regular follow-up appointments with a healthcare provider are important to monitor the progress of spondylolisthesis and adjust treatment as needed.It's crucial for individuals with spondylolisthesis to work closely with healthcare professionals to determine the most appropriate treatment plan based on their unique circumstances. Early diagnosis and intervention can help manage the condition effectively and improve the quality of life for those affected by spondylolisthesis.Risk FactorsSeveral factors increase the risk of developing spondylolisthesis, though it can also occur without any known risk factors:Age: Spondylolisthesis is more commonly observed in adolescents and young adults, with the condition often becoming apparent during growth spurts.Genetics: There may be a genetic predisposition to spondylolisthesis, as it can run in families.Sports Participation: Participation in certain sports that involve repetitive hyperextension of the spine, such as gymnastics, weightlifting, or football, can increase the risk. These activities put stress on the spine, especially in the lower back.Congenital Factors: Some individuals may have congenital abnormalities in the vertebrae that predispose them to spondylolisthesis.Gender: While the condition can affect both genders, some studies suggest that males may be more commonly affected than females.Trauma: Traumatic injuries to the spine, such as fractures, can also lead to spondylolisthesis in some cases.Complications of SpondylolisthesisSpondylolisthesis can lead to various complications, which can vary in severity depending on the degree of vertebral slippage and other factors:Spinal Stenosis: This complication occurs when the spinal canal narrows due to the vertebral slippage, leading to compression of the spinal cord and nerves. Symptoms may include pain, numbness, and weakness in the legs.Nerve Compression: When the displaced vertebrae compress spinal nerves, it can result in symptoms such as sciatica, characterized by pain radiating down the leg, as well as tingling and weakness.Loss of Mobility: Severe cases of spondylolisthesis can significantly limit mobility and quality of life, making daily activities challenging.Bowel or Bladder Dysfunction: Although rare, spondylolisthesis can lead to dysfunction in bowel or bladder control in severe cases.Prevention of SpondylolisthesisPreventing spondylolisthesis is challenging because it is often congenital or develops over time. However, some preventive measures can help reduce the risk or slow down its progression:Maintain a Healthy Weight: Excess body weight can put additional stress on the spine, so maintaining a healthy weight can reduce the risk of spondylolisthesis.Regular Exercise: Engaging in regular physical activity, including exercises that focus on strengthening the core and back muscles, can provide better spinal support.Good Posture: Practicing proper posture and body mechanics, both during daily activities and exercise, can minimize strain on the spine.Nutrition During Pregnancy: Ensuring proper nutrition during pregnancy, including an adequate intake of folic acid, can reduce the risk of congenital spondylolisthesis in infants.Outlook/Prognosis of Spondylolisthesis?The outlook and prognosis of spondylolisthesis depend on several factors, including the severity of the condition, the specific vertebrae affected, the presence of symptoms, and the effectiveness of treatment. Here are some key points regarding the outlook:1. Grades of Spondylolisthesis: Spondylolisthesis is graded based on the degree of vertebral slippage. Grades range from I (mild) to IV (severe). Mild cases (Grade I and II) often have a better prognosis compared to severe cases (Grade III and IV).2. Symptoms: The presence and severity of symptoms significantly impact the prognosis. Some individuals with spondylolisthesis may experience no symptoms or only mild discomfort, while others may have more debilitating symptoms like pain, numbness, or weakness.3. Conservative Treatment: Many cases of spondylolisthesis can be managed conservatively with physical therapy, pain management, and lifestyle modifications. In such cases, individuals can lead relatively normal lives with minimal impact on their daily activities.4. Surgical Intervention: Severe cases or those that do not respond to conservative treatment may require surgical intervention. Surgery can help stabilize the spine and alleviate symptoms. The prognosis after surgery can be positive, but it depends on the surgical technique used and the patient's overall health.5. Complications: Spondylolisthesis can lead to complications such as spinal stenosis or nerve compression. The prognosis may be less favorable if these complications arise and are not adequately managed.6. Lifestyle and Exercise: Engaging in regular exercise and maintaining a healthy lifestyle can improve the prognosis for individuals with spondylolisthesis. Strengthening the core and back muscles can help support the spine and reduce the risk of further slippage.7. Regular Follow-up: Regular medical follow-up and monitoring are essential to track the progress of the condition and adjust treatment as needed.In summary, the outlook for spondylolisthesis varies from person to person and depends on the specific circumstances of the condition. With appropriate treatment and lifestyle management, many individuals can effectively manage spondylolisthesis and lead fulfilling lives. However, severe cases may require more extensive interventions and may have a less favorable prognosis. It's important for individuals with spondylolisthesis to work closely with healthcare professionals to determine the best course of action for their specific situation.
TLIF and Beyond: A Look at Long-term Spinal Health
Transforaminal Lumbar Interbody Fusion (TLIF) is a surgical procedure designed to address specific issues within the spine. During TLIF, surgeons focus on stabilizing and fusing the lumbar (lower back) vertebrae, aiming to alleviate pain and restore spinal integrity.This procedure involves removing a problematic intervertebral disc – the cushion-like structure between adjacent vertebrae – and then fusing the affected vertebrae together. The fusion is typically achieved using a bone graft and, at times, additional hardware like screws and rods to enhance stability.TLIF becomes a viable option when individuals experience persistent back pain or neurological symptoms related to various spinal conditions. These may include degenerative disc disease, where the discs wear down over time, spondylolisthesis, which involves the misalignment of vertebrae, and issues like herniated discs or spinal stenosis.When conservative treatments such as physical therapy or medication fail to provide relief, and diagnostic imaging confirms the severity of the spinal issue, TLIF may be recommended. It's a targeted solution for cases where the spine requires stabilization, nerve decompression, or restoration of disc height to improve overall function and reduce pain.Why TLIF is Done and who needs it?A. Conditions Requiring TLIFDegenerative disc diseaseSpondylolisthesisHerniated discSpinal stenosisB. Purpose of TLIFStabilization of the spineDecompression of nervesRestoration of disc heightTLIF ProcedureA. Preoperative Phase1. Patient Evaluation and PreparationBefore the TLIF procedure, a thorough evaluation of the patient's overall health is conducted. This includes a review of medical history, physical examinations, and assessments of the spine's condition. Any pre-existing health issues that may impact surgery are identified, and preparations are made accordingly.2. Diagnostic Imaging and TestsDiagnostic imaging, such as X-rays, MRI, or CT scans, is crucial for visualizing the specific spinal issues that necessitate TLIF. These images guide the surgeon in planning the surgery, including identifying the location of the affected disc, assessing spinal alignment, and determining the extent of nerve compression.3. Informed ConsentInformed consent is obtained from the patient, ensuring they have a clear understanding of the procedure, potential risks, and expected outcomes. This is a crucial step in promoting patient autonomy and transparency in the medical decision-making process.B. Intraoperative Phase1. Anesthesia AdministrationThe patient is administered anesthesia to induce a state of unconsciousness and painlessness during the surgery. The type of anesthesia (general or regional) is determined based on the patient's health, the complexity of the surgery, and the surgeon's preference.2. Positioning of the PatientThe patient is carefully positioned on the operating table to provide the surgeon with optimal access to the surgical site. Proper positioning is critical for both the safety of the patient and the effectiveness of the procedure.3. Surgical Approach and ExposureThe surgeon makes an incision in the lower back, exposing the affected vertebrae. The choice of the incision and the specific approach (posterior, anterior, or lateral) depends on the patient's condition and the surgeon's expertise.4. Discectomy and Interbody Cage PlacementThe damaged disc material is removed through a process called discectomy. An interbody cage, often filled with bone graft material, is then inserted into the empty disc space. This cage supports the spine, promotes fusion, and helps maintain proper disc height.5. Pedicle Screw PlacementPedicle screws are strategically placed into the vertebrae to provide stability during the fusion process. These screws anchor rods or plates, which further assist in maintaining the alignment of the spine.6. Bone GraftingBone graft material is placed in and around the interbody cage to stimulate bone growth and fusion between the vertebrae. Autografts (patient's own bone), allografts (donor bone), or synthetic grafts may be used, depending on the surgeon's preference and patient factors.C. Postoperative Phase1. Recovery in the HospitalAfter surgery, patients are monitored in the recovery room and then transferred to a hospital room. The initial recovery period involves pain management, observation for any immediate complications, and ensuring the patient is stable before discharge.2. Pain ManagementPain management strategies, including medications and non-pharmacological approaches, are employed to ensure the patient's comfort during the recovery period. This may involve a combination of opioids, nonsteroidal anti-inflammatory drugs (NSAIDs), and physical measures like ice packs.3. Physical Therapy and RehabilitationPhysical therapy is initiated to help patients regain strength, flexibility, and mobility. Specialized exercises are designed to promote healing, prevent complications, and enhance overall spinal function. Rehabilitation plans are tailored to each patient's unique needs.4. Follow-Up AppointmentsRegular follow-up appointments are scheduled to monitor the progress of healing, assess spinal fusion, and address any concerns or complications. Imaging studies may be performed to evaluate the success of the fusion process and the overall stability of the spine.Latest Advancements in TLIF1. Minimally Invasive TLIF TechniquesAdvancements in minimally invasive techniques involve smaller incisions, reduced muscle disruption, and quicker recovery times. Minimally invasive TLIF aims to achieve the same surgical goals while minimizing trauma to surrounding tissues.2. Navigation-Assisted SurgeriesNavigation systems use real-time imaging to guide the surgeon during the procedure. This technology enhances precision in instrument placement, reducing the risk of errors and improving overall surgical outcomes.3. Use of Biologics for Enhanced FusionBiologics, such as growth factors or stem cells, may be used to enhance the bone fusion process. These substances promote the formation of new bone tissue, potentially accelerating the healing and fusion between the vertebrae.Results of TLIFPain Relief: TLIF typically leads to a significant reduction in pain, addressing the root cause of spinal issues and enhancing overall comfort.Improved Spinal Stability: The procedure aims to stabilize the spine, preventing excessive movement between vertebrae and promoting long-term structural integrity.Functional Improvement: TLIF often results in enhanced functionality, allowing individuals to regain mobility and engage in daily activities with increased ease and comfort.Risks and ComplicationsGeneral RisksInfectionBleedingAnesthesia complicationsB. Procedure-specific ComplicationsNerve injuryNonunion or pseudarthrosisStrategies to Prevent ComplicationsInfection prevention protocolsNeurophysiological monitoring during surgeryMinimally invasive techniquesEarly ambulation and strict adherence to postoperative instructionsIn summary, Transforaminal Lumbar Interbody Fusion (TLIF) is a solution for various spinal conditions. While it offers benefits such as pain relief and improved stability, awareness of potential risks is important. Strategic preoperative, intraoperative, and postoperative measures can mitigate complications.

A Guide to Keyhole Spine Surgery
Keyhole Spine Surgery, also known by its more formal names such as Minimally Invasive Spine Surgery (MISS) or Percutaneous Spine Surgery, represents a breakthrough approach in addressing spinal issues with a notably reduced impact on surrounding tissues compared to traditional methods. It's like taking a precision-guided route instead of bulldozing through.In the medical world, you might hear it referred to as Minimally Invasive Spine Surgery (MISS) or Percutaneous Spine Surgery. These monikers essentially highlight the procedure's key characteristic: minimizing invasiveness while achieving effective results.This innovative technique isn't a sudden revelation but rather a product of continuous advancements. Over the years, surgeons have been fine-tuning methods to make spinal surgeries less daunting. Picture it as a journey from more intrusive procedures to ones that can be compared to a keyhole in a door, allowing access without dismantling the entire frame.As technology improved, so did our ability to navigate the intricate landscape of the spine with greater precision. Keyhole Spine Surgery has evolved as a patient-centric response to the desire for quicker recoveries and less postoperative discomfort.Purpose and IndicationsWhy Keyhole Spine Surgery is PerformedAddressing Spinal Issues with Minimal Tissue Disruption:Keyhole Spine Surgery distinguishes itself by minimizing disruption to surrounding tissues. This approach is employed to address spinal concerns without extensive collateral damage.Reducing Postoperative Pain and Recovery Time:The methodology of Keyhole Spine Surgery is designed to reduce postoperative pain and accelerate recovery by minimizing trauma to adjacent tissues. It is an approach focused on efficiency and patient comfort.Patients Who May BenefitDegenerative Disc Disease:Individuals experiencing degenerative disc disease may find Keyhole Spine Surgery beneficial. This procedure aims to address disc issues with a nuanced intervention, avoiding unnecessary disturbance.Herniated Discs:For cases of herniated discs, Keyhole Spine Surgery provides a precise solution without extensive disruption. The approach is analogous to addressing specific disc issues without undue impact on the surrounding area.Spinal Stenosis:Keyhole Spine Surgery is considered for patients with spinal stenosis, a condition characterized by a narrowing spinal canal. The procedure is akin to creating more space without unnecessary alteration.Fractures or Spinal Instability:Cases involving spinal fractures or instability may benefit from the stabilizing nature of Keyhole Spine Surgery. The goal is to provide stability without unnecessary interference with adjacent structures.Tumors:In instances of spinal tumors, Keyhole Spine Surgery allows for precise targeting and removal with minimal disruption to surrounding tissues. It is comparable to a focused approach, minimizing unintended impact during tumor removal.Keyhole Spine Surgery ProcedureBefore SurgeryPatient Evaluation and Selection:Prior to the procedure, a thorough evaluation is conducted to assess the patient's suitability for Keyhole Spine Surgery. This involves considering factors such as overall health, medical history, and the specific spinal condition. It's like ensuring the right tools are chosen for the job.Preoperative Imaging and Diagnostic Tests:Comprehensive preoperative imaging, such as MRI or CT scans, is employed to precisely understand the spinal anatomy. These diagnostic tests serve as a roadmap for the surgical team, ensuring a targeted and accurate approach. It's comparable to studying a map before embarking on a journey.Medication Adjustments and Preparation:Medication adjustments may be necessary before surgery. Patients are guided on any changes required in their medication routine, and preoperative preparations are made to optimize conditions for a successful surgery. It's akin to preparing the ground before planting seeds.During SurgeryAnesthesia Options:Various anesthesia options are discussed with the patient, ranging from general anesthesia to regional or local anesthesia. The choice depends on factors such as the specific procedure and the patient's health. It's like tailoring the comfort level for a customized experience.Positioning of the Patient:The patient is carefully positioned to provide optimal access for the surgical team while ensuring comfort and safety. Think of it as finding the right posture for a task, optimizing efficiency and accessibility.Guidance Tools (Fluoroscopy, Navigation):During surgery, guidance tools such as fluoroscopy and navigation systems are utilized. These tools enhance precision by providing real-time imaging, helping the surgeon navigate with accuracy. It's similar to using GPS for precise navigation.Keyhole Incision and Approach:The procedure involves making a small keyhole incision through which specialized instruments are introduced. This focused approach minimizes disruption to surrounding tissues. It's like using a key to unlock a door rather than dismantling the entire frame.Use of Specialized Instruments (Endoscopes, Microscopes):Specialized instruments, such as endoscopes and microscopes, are employed for enhanced visualization and precision during the surgery. It's comparable to using finely tuned tools for a delicate task.'After SurgeryRecovery in the Hospital:Post-surgery, patients recover in a hospital setting where their condition is monitored. The duration of hospital stay varies based on the specific procedure and individual recovery progress. It's like convalescing in a supportive environment.Postoperative Pain Management:Tailored pain management strategies are implemented to ensure patient comfort. This may include medications and other pain relief techniques. It's akin to providing the right tools for managing discomfort during the recovery phase.Physical Therapy and Rehabilitation:A structured physical therapy and rehabilitation program is initiated to facilitate recovery and restore functionality. This phase is crucial for optimizing long-term outcomes. It's like a personalized training regimen for a complete recovery.Follow-Up Appointments and Monitoring:Regular follow-up appointments are scheduled to monitor recovery progress and address any concerns. This ongoing monitoring ensures the effectiveness of the surgery and facilitates timely interventions if needed. It's like staying connected on a journey to track progress and make adjustments as necessary.Tips for PreparationA. Communication with Healthcare Team:Maintain open and clear communication with your healthcare team.Discuss any concerns or questions about the surgery.Ensure all medications, allergies, and medical history are thoroughly communicated.B. Lifestyle Adjustments Before Surgery:Follow any preoperative instructions provided by your healthcare team.Adjust physical activities as advised.Make necessary lifestyle changes, such as diet adjustments, as recommended.C. Mental Preparation and Support Systems:Seek emotional support from friends and family.Consider counseling or support groups for additional emotional preparation.Engage in relaxation techniques or mindfulness practices to manage stress.Risks and ComplicationsA. General Risks of Surgery:InfectionBleedingReaction to anesthesiaBlood clotsB. Specific Risks Associated with Keyhole Spine Surgery:Nerve injuryInadequate decompression of spinal structuresInfection at the incision siteHardware-related issues (implant malposition or failure)C. Strategies for Risk Prevention:Strict adherence to aseptic techniques to minimize infection risk.Careful preoperative planning and imaging to reduce the risk of inadequate decompression.Monitoring nerve function during surgery to prevent nerve injuries.Choosing appropriate candidates for Keyhole Spine Surgery based on thorough evaluation.Outlook and Prognosis: Keyhole Spine Surgery has positive expectations, notably reducing pain and enhancing functionality, resulting in an improved overall quality of life for patients undergoing the procedure.Successful surgery often prompts patients to consider long-term lifestyle changes. This involves adopting practices such as maintaining a healthy weight, incorporating regular exercise, and adhering to ergonomic principles to ensure sustained spinal health.In conclusion, Keyhole Spine Surgery emerges as a refined and effective approach, providing tailored solutions for various spinal conditions. The emphasis on individualized patient care, coupled with open communication, ensures a more personalized and smoother journey towards recovery.

Herniated Discs: Risk Factors, Prevention Strategies, and Nutrition
Herniated disc is like when the soft, jelly-like part of a spinal disc decides it wants to explore the outside world, pushing through a weakened spot in its protective ring. We also call it a slipped or ruptured disc. Fancy names for a not-so-fancy situation.And guess what? When this happens, it can bring along a posse of unpleasant sensations like pain, numbness, or weakness in your arm or leg. Not exactly the kind of adventure you signed up for, right?Now, here's the deal: to keep your spine happy and pain-free, you need to be buddies with three key things—understanding the risks, keeping preventions on your radar, and showing some love to your body through nutrition.Risk Factors for Herniated Discs:1. Age:Think of your spinal discs like well-worn tires. As we age, they don't get younger. The wear and tear add up, making the chances of herniated discs more likely. It's the natural course of the road, but knowing it helps you steer wisely.2. Genetics: Family ties are strong, and so are genetic links. If herniated discs are a family affair, it's like a warning sign. Extra caution is your way of putting on a seatbelt for your spine.3. Occupation and Lifestyle: Your daily grind can have a big say in your spine's well-being. Jobs that involve heavy lifting or constant twisting are like road bumps for your spine. Being mindful of your work-related activities is your way of paving a smoother path.4. Weight: Carrying excess weight isn’t just about appearance; it's a load your spine has to bear. Picture it like a backpack—those extra pounds stress your spine. Maintaining a healthy weight is like taking off the unnecessary load.5. Smoking: Smoking isn’t just a hazard for your lungs; it's like sending a smoke signal to your discs. Reduced oxygen supply is like giving your discs a foggy day. Quitting smoking is like opening up a clear pathway for your spine to breathe.Understanding these risks is like having a map for your spinal journey. It helps you anticipate the twists and turns, making informed decisions to keep your spine on the smoothest route possible. So, age gracefully, know your genetic roadmap, be kind to your spine at work, shed that extra weight, and let your spine breathe by ditching the smoke. Your back will thank you for the thoughtful navigation! Strategies to Keep Your Back Happy1. Proper Lifting Techniques: When you lift stuff, channel your inner superhero by using your legs, not your back. Bend those knees and keep whatever you're lifting close. It’s not just a lift; it's a dance move for your spine’s well-being.2. Maintain a Healthy Weight: Picture your spine as your personal sidekick. Eat balanced meals and get moving regularly—it’s like giving your spine a superhero suit. Managing your weight is your way of being a sidekick to your spine’s superhero adventures.3. Regular Exercise: Strengthen that core—it's your spine's daily workout. Whether you're into the zen of yoga or the punch of Pilates, these exercises are like high-fives for your spinal health. Think of it as a gym membership for your spine.4. Proper Ergonomics: Your workspace and home are like cozy nests for your spine. Make them comfy and ergonomic—it's like a spa day for your back. Good posture isn't just for photos; it's a daily gift to your spine, making it feel right at home.5. Quit smoking: If smoking is part of your routine, consider mixing it up. Quitting isn't just about your lungs; it’s like opening the windows for your discs. Better circulation is like a breath of fresh air for your spine.these are just friendly tips to keep your back feeling happy and healthy. Lift like a pro, eat well, move often, make your surroundings spine-friendly, and if you smoke, consider giving it a break. Your spine is on a lifelong journey with you, so let’s make it a pleasant one! Nutrition and Herniated Discs:1. Calcium and Vitamin D:These as the superheroes for your bones, especially the vertebrae in your spine. They team up to keep your bones strong and healthy.Say hello to dairy products—milk, cheese, and yogurt are your buddies. Leafy greens like kale and spinach also make the list. And don’t forget the sunshine; it’s a natural source of vitamin D.2. Omega-3 Fatty Acids:Meet the inflammation fighters. These fatty acids, found in fatty fish like salmon, flaxseeds, and walnuts, can help keep inflammation at bay, which is excellent news for your discs.Dive into a plate of grilled salmon, sprinkle some flaxseeds on your yogurt, or munch on a handful of walnuts for a tasty dose of omega-3 goodness.3. Collagen:Collagen is like the glue that holds things together, especially your connective tissues, including those discs in your spine. It's the support system you didn’t know you needed.Sip on some comforting bone broth, indulge in chicken or fish dishes, or consider collagen supplements for an extra boost.4. Hydration:Water is the unsung hero. Staying well-hydrated is like giving your discs a drink. It maintains the water content in your spinal discs, keeping them flexible and ready for action.Sip water throughout the day. Make it a habit to carry a reusable water bottle, and your spine will thank you.5. Anti-inflammatory Foods:Berries, turmeric, and ginger are like your personal army against inflammation. They contain antioxidants and anti-inflammatory properties that can soothe your spine and keep it happy.Toss a handful of berries into your morning cereal, sprinkle some turmeric on your veggies, or brew a ginger tea for a delicious and spine-friendly treat.In a nutshell, your spine loves a good mix of nutrients. So, include a variety of foods in your diet, from the calcium-rich dairy to the omega-3-packed fish, collagen-boosting options, and inflammation-fighting goodies. Your spine will thank you for the extra care and attention!






